Understanding Late Night Leg Cramps: Causes and Solutions


Intro
Late night leg cramps can be a frustrating experience for many individuals. These sudden and involuntary contractions of the muscles in the legs often occur during sleep, causing discomfort and disruption. Understanding the underlying causes of these cramps is essential for effective management and prevention. Multiple factors can contribute to this condition, including hydration status, dietary habits, physical activity levels, and overall health.
In this article, we delve into these causes, disbursing myths and highlighting crucial insights for health professionals, wellness coaches, nutritionists, fitness trainers, and mindfulness instructors. By grasping these elements, one can potentially mitigate the risk of late night leg cramps and promote better health outcomes.
Wellness Insights
Benefits of Regular Exercise
Engaging in regular physical activity plays a significant role in maintaining muscle function and reducing the likelihood of cramping. Exercise stimulates blood circulation, which is essential for muscle health. Strengthening the muscles through various forms of workouts can also enhance flexibility. This flexibility is crucial in preventing muscle tightness, one of the potential causes of leg cramps.
Here are a few ways regular exercise can help:
- Improves circulation: Enhanced blood flow ensures that muscles receive necessary oxygen and nutrients.
- Increases flexibility: Stretching and strength training can prevent tightness.
- Boosts overall health: A physically active lifestyle supports metabolic functions, reduces stress, and helps maintain healthy body weight.
Understanding Mental Health
Mental well-being can impact the frequency and intensity of leg cramps. Stress and anxiety can lead to muscle tension. When the body is in a heightened state of arousal, it may not relax properly during sleep, leading to cramps.
Practicing mindfulness and relaxation techniques can assist in managing both mental health and muscle relaxation. Some effective strategies include:
- Meditation: Calming the mind can relieve bodily tension.
- Deep-breathing exercises: These can lower stress levels and promote relaxation.
- Yoga: Incorporating yoga into a daily routine may enhance flexibility and mental clarity.
"Understanding the connection between mental health and physical manifestations such as leg cramps can lead to more holistic treatment approaches."
Nutrition Information
Balanced Diet Essentials
A balanced diet is crucial for preventing late night leg cramps. Nutrients such as potassium, magnesium, calcium, and sodium are vital for muscle contraction and relaxation. When these electrolytes are out of balance, muscle cramps may occur. Ensuring adequate intake of these nutrients is essential.
Foods rich in these electrolytes include:
- Potassium: Bananas, oranges, and spinach.
- Magnesium: Nuts, seeds, and whole grains.
- Calcium: Dairy products, leafy greens, and tofu.
- Sodium: Table salt, seafood, and processed foods (in moderation).
Meal Planning and Preparation
Implementing practical meal planning can assist in addressing nutritional needs. Preparing meals in advance ensures that individuals consume essential vitamins and minerals regularly. It can also reduce reliance on convenience foods, which often lack essential nutrients.
Here are tips for effective meal planning:
- Create a weekly menu: This helps organize shopping and ensures a balanced intake of nutrients.
- Batch cooking: Preparing larger portions can save time and maintain nutritional balance.
- Include a variety of foods: A diverse diet maximizes nutrient intake.
Prelims to Late Night Leg Cramps
Late night leg cramps are a common issue that can significantly disrupt sleep and cause discomfort. Understanding the causes behind these cramps is essential not only for relief but also for prevention. The involuntary contractions usually occur during the night, affecting sleep quality and daily functioning. The focus of this article will be to dive deep into this phenomenon, outlining the various factors contributing to leg cramps.
The importance of grasping the underlying mechanisms of these cramps cannot be understated. The explanations range from physiological aspects to lifestyle factors. Recognizing these elements helps health professionals and individuals who encounter such issues to take proactive steps in their management.
Defining Leg Cramps
Leg cramps are sudden, involuntary contractions of one or more muscles. They can last for a few seconds to several minutes, often resulting in sharp pain. While any muscle can cramp, calf muscles are particularly susceptible. The nature of these contractions differs from typical muscle tightness or soreness.
Leg cramps that occur at night are usually referred to as nocturnal leg cramps. They might be experienced by anyone, but their characteristics, frequency, and trigger vary. Understanding this definition lays the groundwork for identifying effective strategies to mitigate their occurrence.
Prevalence of Late Night Leg Cramps
The prevalence of late night leg cramps is significant, affecting a substantial number of individuals, especially those over the age of 50. Though often benign, they can severely impact sleep and overall well-being. Research shows various statistics indicating that up to 60% of older adults report experiencing nocturnal leg cramps at least once in a month.
Factors contributing to this high prevalence include:
- Increased muscle fatigue due to aging
- Greater sedentary lifestyles
- Dietary insufficiencies in key nutrients
Furthermore, people involved in physical activities might experience occasional cramps as a consequence of muscle fatigue or dehydration. The widespread nature of this problem underscores the necessity for effective assessment and intervention strategies.
Physiological Mechanisms of Cramps
Understanding the physiological mechanisms of cramps is essential for comprehending the complexities behind late night leg cramps. This section sheds light on how the body's systems interact to produce these involuntary muscle contractions. Insight into these mechanisms is valuable for health professionals, wellness coaches, and others who seek to manage or prevent cramps effectively. This knowledge enables a more precise approach, tailoring advice for individuals based on their unique physiological makeup.
Muscle Physiology Overview
Muscle cramps primarily stem from the contraction of skeletal muscles. Skeletal muscles operate through a delicate balance of signals from the nervous system and biochemical processes within the muscle fibers. When a muscle is stimulated, a cascade of events begins. Calcium ions are released within the muscle cells, triggering contraction. Normally, this process is tightly regulated, allowing for smooth and coordinated movements. However, disturbances—due to fatigue, dehydration, or electrolyte imbalances—can lead to dysfunction.
When fatigue sets in, the muscles may become overexcited, sometimes resulting in sustained contractions. Much of the body's physiology relies on homeostasis. As muscles tire, they may lose their ability to relax, leading to cramps. A clear understanding of these physiological properties is beneficial for those addressing issues of muscle health and functionality.
Neuromuscular Factors
Neuromuscular factors play a significant role in muscle cramps. The relationship between nerves and muscles is essential for proper movement and function. Nerve signals direct muscle contractions, and any dysfunction can affect this communication. Conditions affecting the nervous system, like neuropathy or nerve compression, can result in cramps.
Factors such as stress, anxiety, and fatigue alter the neuromuscular dynamics. For instance, stress may lead to heightened neural excitability, increasing susceptibility to cramps. Similarly, if the central nervous system is overloaded, it can cause disruption in muscle control, leading to involuntary contractions.
A deep understanding of neuromuscular factors highlights the need for holistic approaches in managing cramps. This includes stress management, proper hydration, and emphasis on relaxation techniques to support the neuromuscular junction’s efficacy. By prioritizing these elements, professionals can give better guidance on mitigating muscle cramps.
"Understanding the interplay between physiological mechanisms and neuromuscular factors can empower individuals to develop effective strategies for managing late night leg cramps."
Recognizing these underlying mechanisms equips health professionals and coaches with the tools necessary for effective interventions.
Dehydration and Its Role
Dehydration plays a significant role in the occurrence of late night leg cramps. It is crucial to understand how fluid balance impacts muscle function. The body relies on a combination of water and electrolytes to maintain optimal cellular performance and contraction. Insufficient hydration can lead to a cascade of effects that contribute to muscle cramps, influencing both the frequency and severity of these issues.
Understanding Dehydration
Dehydration occurs when the body loses more fluids than it takes in. This can happen for various reasons, including rigorous physical activity, high temperatures, or simply not drinking enough water throughout the day. The symptoms can range from mild to severe, including dryness of the mouth, fatigue, dizziness, and muscle cramps.
- Types of dehydration: There are primarily two types: isotonic and hypertonic. Isotonic dehydration involves losing both water and electrolytes equally, while hypertonic dehydration typically involves a greater loss of water compared to electrolytes, leading to an imbalance.
- Signs to watch for: Common indicators include:
- Thirst
- Decreased urine output
- Dark-colored urine
- Fatigue
Recognizing these signs can aid in effective fluid management before muscle cramps occur.
Link between Dehydration and Muscle Cramps


The connection between dehydration and muscle cramps is well-documented. When the body is dehydrated, it can affect the regulation of neurotransmitters and the overall muscle function. Low fluid levels can lead to increased muscle excitability and contractions. This results in heightened susceptibility to cramps, especially during periods of rest, such as when one is trying to sleep.
- Electrolyte Disruption: Key electrolytes like sodium, potassium, and calcium play pivotal roles in muscle contraction and relaxation. Dehydration can disrupt the balance of these electrolytes, making it harder for muscles to respond appropriately.
- Muscle Cramps: Cramps can manifest as sudden, involuntary contractions, often in the calf muscles. These are not only painful but can interfere with sleep quality.
"Maintaining proper hydration is essential for muscle performance, especially during and after exercise. Avoiding dehydration may significantly reduce the occurrence of late-night leg cramps."
In summary, recognizing and addressing dehydration is vital in mitigating leg cramps. Adequate hydration enhances muscle function and can lead to better sleep quality by reducing involuntary muscle contractions.
Electrolyte Imbalances
Electrolyte imbalances play a crucial role in understanding late night leg cramps. These imbalances disrupt normal muscle function, leading to involuntary contractions that can cause pain and discomfort during the night. Electrolytes are minerals in the body that carry an electric charge. They are vital for various physiological processes, including muscle contractions, nerve function, and hydration.
Proper levels of electrolytes such as sodium, potassium, calcium, and magnesium are essential for maintaining muscle health. An understanding of these components helps shed light on why cramps may occur, their prevention, and potential solutions to address them effectively.
Key Electrolytes Involved
Several key electrolytes are critical in preventing leg cramps:
- Sodium: Affects fluid balance and muscle function. It helps regulate blood pressure and is crucial when exercising.
- Potassium: Plays a significant role in muscle contractions and maintaining healthy nerve function. Insufficient potassium levels can lead to cramps during physical activities or at rest.
- Calcium: Necessary for muscle contraction. Low calcium levels can disrupt the balance needed for proper muscle function, resulting in cramps.
- Magnesium: Facilitates muscle relaxation and contraction. A deficiency can lead to excessive muscle contractions, linking it closely to the occurrence of cramps.
Each of these electrolytes needs to be balanced to ensure optimum muscle and overall bodily functions.
Impact of Imbalances on Muscle Function
Electrolyte imbalances can significantly affect muscle function. When certain electrolytes are either deficient or excessive, muscle contractions can become irregular. Here are some key impacts:
- Decreased Muscle Performance: Low levels of potassium and magnesium can hinder muscle contractions, making it difficult for muscles to relax properly.
- Increased Cramps: With low calcium or potassium levels, the risk of cramps rises, especially during night time when the body is at rest.
- Altered Nerve Signals: Imbalances also affect the transmission of nerve signals, leading to confusion in the messages sent to muscles, resulting in involuntary contractions.
Understanding how these electrolytes function can guide effective prevention and management strategies for those who experience late night leg cramps. Tackling electrolyte imbalances through nutrition or supplementation may offer relief and improve overall muscle health.
Muscle Fatigue and Overuse
Muscle fatigue and overuse are critical factors in understanding late night leg cramps. These cramps often stem from an imbalance in physical exertion and recovery. Recognizing the signs of muscle fatigue can help prevent discomfort, reduce the frequency of cramps, and improve overall muscle health. This topic draws attention to how cumulative exertion affects muscle function and recovery, emphasizing the need for proper management strategies.
Understanding Muscle Fatigue
Muscle fatigue refers to the temporary inability of a muscle to maintain its normal strength and performance. This condition can arise from a variety of factors, including prolonged physical activity and insufficient recovery methods. Fatigue is particularly relevant in the context of leg cramps, as it can lead to the overstimulation of muscle fibers.
Key points to consider about muscle fatigue include:
- Causes: It may result from the depletion of energy stores, leading to insufficient ATP production responsible for muscle contractions.
- Symptoms: Common symptoms include a sense of heaviness, weakness, and reduced endurance, which can exacerbate leg cramp episodes at night.
- Recovery Needs: Adequate rest and nutrition are critical in the recovery process to restore energy levels and mitigate the risk of cramps.
Regular assessments of fatigue levels and an understanding of how the body responds to exertion can aid in preventing cramps and promoting muscle health. Monitoring how your body reacts to various activities allows for informed adjustments to exercise routines.
Overexertion in Physical Activities
Overexertion, defined as engaging in physical activities beyond the body's capacity to recover, is a prevalent cause of late night leg cramps. This often occurs in individuals who push their limits during exercise, neglecting the signs of fatigue and stress in their muscles.
Overexertion poses several considerations for muscle health:
- Training Programs: A well-balanced training program with gradual increases in intensity can help avoid muscle overuse.
- Rest and Recovery: Incorporating proper rest days into fitness routines is essential. Neglecting recovery not only increases the likelihood of cramps but also hinders long-term performance.
- Listening to Your Body: Being attentive to physical signals, such as pain or excessive fatigue, can help to prevent overuse injuries and cramping episodes.
To minimize the risks associated with overexertion, it is essential to maintain a balanced fitness regimen that prioritizes both challenge and recovery.
By understanding the relationship between muscle fatigue, overuse, and late night leg cramps, individuals can develop better strategies for their physical activities, ultimately leading to improved performance and well-being.
Impact of Sedentary Lifestyle
Sedentary lifestyle is a significant factor when exploring the causes of late night leg cramps. A lifestyle that lacks physical activity can contribute to various health conditions that manifest in muscle cramps. Inactivity leads to muscle weakness and stiffness, making them more susceptible to spasms during rest periods.
Prolonged periods of sitting can alter normal muscle function. The muscles, when not engaged regularly, can lose their endurance and become more prone to fatigue. This is particularly true for leg muscles, which support the weight of the body and endure considerable strain during daily activities. Not engaging these muscles results in poor circulation and can exacerbate cramping episodes.
Consequences of Inactivity
Inactivity carries several repercussions that can directly impact muscle function:
- Muscle Deconditioning: Regular movement keeps muscles conditioned and responsive. Lack of activity leads to deconditioning, making muscles less capable of handling physical stress.
- Poor Circulation: Sitting for extended periods limits blood flow. This can lead to further issues as nutrients and oxygen become less available to muscle tissue.
- Increased Incidence of Conditions: Conditions like obesity and diabetes can emerge from a sedentary lifestyle, both of which have been linked to higher rates of leg cramps.
"Regular physical activity is crucial for maintaining muscle health and function, ensuring better leg performance during the night."
Insufficient Range of Motion
An insufficient range of motion exacerbates the issue of late night leg cramps. When physical activity is low, joints and muscles may not stretch adequately. This lack of use can result in shortened muscles and tightness, increasing the risk of cramps during sleep. Adequate stretching and mobility exercises are often neglected in a sedentary lifestyle. Incorporating dynamic stretches can enhance flexibility in muscles and joints, reducing the incidence of cramps.
To mitigate these risks, it is essential to recognize the importance of integrating physical activity into daily routines. This can include simple adjustments such as taking short walks, practicing stretches, or engaging in strength training. All of these actions promote better circulation and muscle health, ideally reducing the likelihood of late night leg cramps.
Age and Musculoskeletal Changes
Understanding the impact of age on musculoskeletal health is vital in the context of late night leg cramps. As people age, their muscle composition and overall joint health tend to decline. This deterioration can explain why older adults frequently experience these muscle spasms during the night. Not only does age bring about physical changes, but it also interacts with other factors such as hydration and nutrition. This section aims to shed light on these specific elements and how they relate to cramping.
Aging and Muscle Mass
Aging significantly affects muscle mass, often leading to sarcopenia, which is the gradual loss of muscle tissue. This occurs due to a combination of hormonal changes, reduced physical activity, and the body’s decreased ability to synthesize proteins. The loss of muscle mass can weaken the muscles in the legs, making them more susceptible to cramps at night.
Moreover, these muscle changes can lead to decreased endurance and strength. When leg muscles become weaker, they may struggle to support basic functions such as walking or standing. The overuse of these weaker muscles, especially during the day, can contribute to fatigue and ultimately result in leg cramps at night. Maintaining an active lifestyle and engaging in resistance training can help slow muscle degeneration, but many older adults find it challenging to stick to such routines.
Joint and Muscle Health Decline
The decline in joint and muscle health is another critical aspect of aging that influences late night leg cramps. Over time, cartilage cushioning in joints wears down, leading to conditions such as osteoarthritis. This deterioration not only causes pain but can affect mobility. Individuals may experience stiffness in their joints, which impacts their ability to stretch or move their muscles properly.
When muscles are not properly engaged or stretched, they can seize up and lead to cramps. The relationship between joint and muscle health is profound, as one often influences the other. Individuals with joint issues may unknowingly alter their movement patterns, generating more stress on their muscles and increasing the likelihood of cramps.
"The decline in muscle mass and joint health is intertwined; neglected joints can lead to muscular discomfort, especially at night."
Combating these effects requires attention to both nutrition and exercise. Ensuring adequate intake of key nutrients, such as calcium and vitamin D, can help maintain muscle and bone health. Additionally, regular low-impact activities, such as swimming or cycling, can improve joint function without overstraining the body.
Overall, addressing the challenges posed by aging involves a multi-faceted approach that considers both muscle mass and joint integrity. Both factors are essential for understanding the occurrence of late night leg cramps in older individuals.
Underlying Health Conditions
Understanding the underlying health conditions that may contribute to late night leg cramps is critical for both prevention and management. Numerous health issues can increase the likelihood of experiencing these cramps. Identifying these conditions allows individuals to make informed decisions and take proactive steps toward alleviating symptoms. Addressing the root causes can lead to improved muscle function and overall better health outcomes.
Diabetes and Related Complications
Diabetes is a significant factor often associated with late night leg cramps. This chronic condition may result in nerve damage, known as diabetic neuropathy. This damage affects the nerves, which can lead to unsought contractions of muscles. High blood sugar levels may also impact circulation, reducing blood flow to the legs and exacerbating cramping.
Moreover, managing diabetes effectively is crucial to mitigate related complications. Regular monitoring of blood sugar levels, maintaining a balanced diet, and following prescribed medication regimens can help keep these cramps at bay. Patients with diabetes should also consult healthcare professionals if they notice an increase in frequency or intensity of leg cramps.
Peripheral Artery Disease
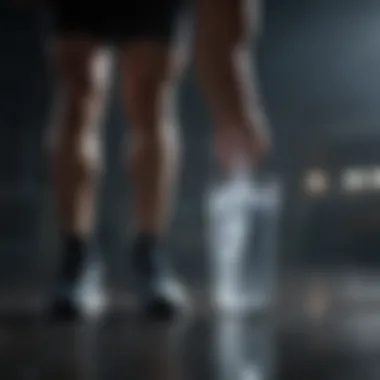

Peripheral artery disease (PAD) is another health issue that can lead to late night leg cramps. PAD involves narrowing of the arteries, which reduces blood flow to the limbs. This reduced blood flow can cause muscle cramping, especially during physical activity or during rest at night. Individuals with PAD may experience discomfort or cramping in their legs due to insufficient oxygen supply to the muscles.
Managing PAD through lifestyle changes is essential. This includes regular exercise, proper nutrition, and, in some cases, medication. Understanding how PAD affects circulation is important for recognizing its link to leg cramps. Individuals should seek medical advice regarding PAD management strategies to avoid complications.
Other Contributing Conditions
Several other health conditions may also contribute to occurrences of late night leg cramps. Conditions such as hypothyroidism, kidney disease, and multiple sclerosis can have similar effects on muscle function and nerve health.
- Hypothyroidism: An underactive thyroid can lead to muscle weakness, which may increase the risk of cramping.
- Kidney Disease: Poor kidney function can disrupt the balance of electrolytes, further contributing to cramps.
- Multiple Sclerosis: This neurological disorder may also affect nerve function, leading to muscle spasms, including cramps at night.
It is beneficial for individuals experiencing frequent leg cramps to evaluate their overall health status. Engaging in routine check-ups and seeking advice from healthcare providers can inform assessments of risks and management of any underlying conditions contributing to cramps.
"Addressing underlying health conditions is key to understanding the cause of late night leg cramps and fostering better health performance overall."
Recognizing these medical factors is an essential step towards understanding late night leg cramps better. It fosters a comprehensive approach that combines lifestyle adjustments with medical insights to help manage this often troubling issue.
Medication Effects
Medications can play a significant role in the occurrence of late night leg cramps. Understanding how these medications affect muscle function and overall health is essential for anyone experiencing muscle cramps during the night. It is important for health professionals, wellness coaches, nutritionists, fitness trainers, and mindfulness instructors to be aware of this topic as it can influence their approach to management and prevention strategies. Identifying the right medications and understanding their impacts can help in developing effective treatment plans and improving the quality of life for individuals suffering from cramps.
Common Medications Linked to Cramps
Several types of medications have been associated with leg cramps. Here are key categories and examples:
- Diuretics: Drugs like furosemide and hydrochlorothiazide are often prescribed for hypertension. They can lead to electrolyte depletion, which may contribute to cramping.
- Statins: Medications such as atorvastatin or simvastatin can cause muscle pain and cramps as a side effect.
- Hormonal Therapies: Treatments including testosterone replacement therapy and estrogen can also influence muscle function and increase the likelihood of cramps.
- Antipsychotics: Certain drugs like haloperidol have been linked to muscle cramps as a side effect.
Understanding these medications allows for better assessment of their risks and benefits, especially for those who experience late night leg cramps.
Mechanisms of Impact
The mechanisms by which medications induce leg cramps can be multifactorial. Here are some critical aspects:
- Electrolyte Disruption: Many medications, especially diuretics, can cause dehydration or electrolyte imbalance. This imbalance often results in low potassium, calcium, or magnesium levels. Such deficiencies are significant contributors to muscle cramps.
- Muscle Relaxation and Stress: Some medications might alter neuromuscular transmission. For example, certain antipsychotic medications impact neurotransmitter levels, which could affect muscle tone and lead to cramping.
- Increased Muscle Tension: Statins, while effective for cholesterol control, may disrupt normal muscle metabolism, leading to muscle stiffness or cramps. The mechanism involves the inhibition of cholesterol production, affecting cell membranes and overall muscle function.
These mechanism details provide insight into how medications directly or indirectly cause cramping, emphasizing the need for careful monitoring of individuals prescribed such treatments.
"Understanding the potential side effects of medications is crucial in developing holistic management strategies to minimize leg cramps and enhance muscle function."
In summary, the effects of medication on leg cramps cannot be overlooked. Awareness of common medications and their impact mechanisms is key for professionals involved in patient care and wellness. A detailed understanding of these aspects will facilitate more informed decisions, leading to improved outcomes for individuals suffering from late night leg cramps.
Nutritional Deficiencies
Nutritional deficiencies play a significant role in the onset of late night leg cramps. Insufficient intake of key vitamins and minerals can contribute to these involuntary muscle contractions. This section explores the specific nutrients essential for proper muscle function, their sources, and the consequences of their absence in one’s diet. Understanding these elements aids individuals in taking proactive measures against cramps.
Key Nutrients Affecting Muscle Function
Several key nutrients directly influence muscle contractility, including potassium, magnesium, calcium, and sodium. Each of these plays a distinct role:
- Potassium: Essential for the proper functioning of cells, potassium aids in muscle contractions. Low levels can lead to weakness and cramps.
- Magnesium: This mineral helps muscles relax and prevents overcontraction. A deficiency can result in increased muscle tension.
- Calcium: Critical for muscle contraction, calcium levels need to be properly regulated within the bloodstream. Imbalances may result in unwarranted cramps at night.
- Sodium: While often overlooked, sodium regulates fluid balance. A shortage can lead to dehydration, compounding the risk of cramps.
"Adequate intake of these nutrients can dramatically reduce the frequency of leg cramps, especially during the night."
Thus, maintaining sufficient levels of these nutrients is vital in preventing late night leg cramps, and allows muscles to function smoothly.
Sources of Essential Nutrients
The quality of our diet directly impacts the levels of these essential nutrients. Here are some rich sources of each:
- Potassium: Available in bananas, avocados, and sweet potatoes. Leafy greens also offer a good amount.
- Magnesium: Found in nuts, seeds, whole grains, and dark chocolate. Green leafy vegetables are another option.
- Calcium: Dairy products like milk, cheese, and yogurt are well known for calcium. Fortified plant-based milks also provide it.
- Sodium: While it can be obtained from table salt, processed foods often contain high amounts, making it easy to consume adequately.
Incorporating a variety of these foods into the daily diet can support muscle function and help prevent nighttime leg cramps. A little attention to nutrition can offer significant relief.
Genetic Factors
Genetic factors can significantly influence the likelihood and severity of late night leg cramps. Understanding these elements is crucial for health professionals, wellness coaches, and individuals affected by this condition. Genetic predisposition may determine how muscle function and electrolyte balance is regulated in the body, which can ultimately affect the occurrence of muscle cramps during sleep.
Hereditary Tendencies
Research has demonstrated that certain individuals may inherit a higher tendency to experience leg cramps. This hereditary aspect can encompass variations in muscle fiber composition, neuromuscular transmission, and even differences in hydration and electrolyte processing capabilities. Families may observe patterns where multiple members experience similar discomfort, suggesting a genetic link.
- Muscle Fiber Types: Some people may have a higher proportion of fast-twitch muscle fibers, which have been associated with a greater risk of cramps.
- Neuromuscular Factors: Genetic variations can affect how muscles react to nerve signals, potentially leading to involuntary contractions.
- Electrolyte Management: Differences in how the body retains or expels electrolytes could make certain individuals more prone to imbalances, exacerbating cramping issues.
Research on Genetic Contributions
Ongoing studies aim to clarify the genetic underpinnings of leg cramps, focusing on specific genes that may play a role in muscle contraction and relaxation. Research findings indicate that candidate genes associated with neuromuscular function can impact susceptibility to cramps. Variants in these genes might lead to altered muscle mechanics or impaired neuromuscular control, resulting in increased occurrences of cramps during the night.
"Integrating genetic insights can enhance our understanding of late night leg cramps, allowing for tailored management strategies."
Additionally, understanding these genetic contributions could pave the way for personalized prevention methods. For instance, individuals with a family history of cramps may benefit from targeted nutritional strategies or monitored exercise regimens designed to mitigate symptoms. Future research may also explore how genetic information can inform professional advice, offering bespoke solutions for those prone to night-time cramps.
By shedding light on the genetic factors that affect leg cramps, individuals can become more empowered to recognize their risks and take proactive measures to manage their condition.
Lifestyle Choices
Lifestyle choices play a pivotal role in understanding late night leg cramps. Numerous factors ranging from daily habits to overall physical activity can influence the frequency and severity of these cramps. Addressing lifestyle choices can empower individuals to potentially mitigate cramps and enhance their quality of sleep.
Habits That May Contribute
Several daily habits can exacerbate the occurrence of leg cramps. For instance, lack of physical activity is a significant contributor. Sedentary behavior leads to muscle weakens and reduced flexibility, increasing the likelihood of cramps during rest. Furthermore, poor hydration practices can worsen the situation. Many individuals fail to drink enough water throughout the day, leading to dehydration, which has been linked to muscle cramping.
Additionally, excessive consumption of caffeine or alcohol can negatively impact muscle function. Caffeine is a stimulant and may increase muscle excitability, while alcohol can act as a diuretic and lead to fluid loss. Balancing these habits is essential for reducing the risk of cramps.
"Adjusting daily routines can provide significant relief from discomfort and enhance overall well-being."
Dietary choices also come into play. Consuming a well-balanced diet rich in vitamins and minerals helps maintain muscle function. Deficiencies in nutrients like magnesium or potassium may trigger or worsen cramps. Increasing the intake of vegetables, fruits, whole grains, and lean proteins is beneficial.
Sleep Position and Its Effects
The position one chooses for sleeping may significantly affect the occurrence of leg cramps. Certain sleeping postures can place undue stress on the muscles, leading to contractions. For example, sleeping with feet pointed downward can tighten the calf muscles, which can initiate a cramp. It’s advisable to maintain a more neutral carpet position to avoid unnecessary strain.
Using proper supportive pillows or cushions can improve sleep positions and help maintain aligned lower limbs. Stretching or performing relaxation techniques before bed can also mitigate the risk of cramps. Incorporating a short routine that includes gentle leg stretches or yoga can greatly enhance muscle relaxation and flexibility.
In summary, by making informed lifestyle choices, individuals can better manage the incidence of late night leg cramps. Being aware of daily habits and sleep positions empowers individuals to take action toward improving their sleep quality.
Carefully observing one’s routines can reveal hidden contributors to discomfort, making it easier to adjust for better health.

Recognizing Early Symptoms
Recognizing early symptoms of late night leg cramps is crucial for effectively managing and preventing future occurrences. Understanding the signs allows individuals to take proactive measures that can mitigate discomfort and improve overall sleep quality. When symptoms are identified early, it may reduce the impact of cramps on one's life, allowing for more restful nights and better day-to-day functioning.
Identifying Cramps vs. Other Conditions
Differentiating leg cramps from other potential medical issues is essential. Symptoms can sometimes overlap with conditions like restless leg syndrome or circulatory problems. A cramp typically presents as a sudden, involuntary contraction of the muscle, often felt as a sharp, intense pain. Conversely, restless leg syndrome involves an urge to move the legs accompanied by uncomfortable sensations but does not generally present with the intense pain associated with cramps.
Some effective methods for identifying cramps include:
- Observing the onset and duration of the pain. Leg cramps usually last from several seconds to a few minutes.
- Noting specific triggers. Cramps often happen during rest, especially at night, whereas other conditions may have different triggers.
- Recognizing muscle involvement. Cramps often occur in the calf, thigh, or foot muscles, while other conditions might affect multiple areas of the body.
Common Indicators of Cramps
Awareness of common indicators can enhance understanding of this phenomenon. Recognizable signs include:
- Sudden onset of pain in the leg muscles that may be intense and localized.
- A noticeable hardening or tightness of the muscle during the episode.
- Occurrences that usually take place during the night while the individual is at rest.
- Pain that resolves with stretching of the muscle or moving the legs, contrasting with other painful conditions that may not respond as quickly.
Being aware of the patterns related to cramps can aid individuals in discussing their symptoms with healthcare providers, potentially leading to better management strategies.
Understanding the early signs of leg cramps is essential. By distinguishing cramps from other conditions and recognizing key indicators, individuals can more effectively approach relief and prevention.
Prevention Strategies
Understanding the prevention strategies for late night leg cramps is essential. These cramps can disturb sleep and lead to unnecessary discomfort. Implementing effective strategies can reduce their occurrence and improve overall well-being. Main aspects include proper hydration, nutrition, tailored exercise, and lifestyle adjustments.
Hydration and Nutrition Tips
Hydration is a core component in preventing leg cramps. Keeping the body adequately hydrated ensures that muscles have enough fluid to function efficiently. Water plays a vital role in muscle contraction and relaxation. Therefore, drinking sufficient water throughout the day is crucial to managing dehydration.
Nutritional intake is equally vital. Specific nutrients significantly affect muscle function:
- Potassium: Found in bananas, oranges, and potatoes, potassium helps maintain muscle health.
- Magnesium: Present in leafy greens, nuts, and whole grains, magnesium is critical in reducing muscle cramps.
- Calcium: Important for muscle contractions, calcium can be sourced from dairy products and fortified plant-based alternatives.
It is beneficial to integrate a balanced diet to ensure the essential nutrients are consumed. Aim for a variety of foods that contain these key nutrients to support muscle function and overall health.
Exercise and Flexibility Routines
Incorporating regular exercise is important in preventing late night leg cramps. Engaging in physical activity strengthens muscles and improves endurance. However, it is vital to choose exercises that are appropriate for your fitness level.
Flexibility routines can be particularly effective. Stretching before bedtime can ease muscle tension. Specific stretches to focus on include:
- Calf Stretch: Stand facing a wall, with one foot behind the other, and press the heel of the back foot into the ground.
- Hamstring Stretch: Sit with one leg extended, reach toward your toes, holding the stretch gently.
"Regular flexibility training not only prevents cramps but also enhances overall muscle performance."
Additionally, engaging in activities such as yoga can improve flexibility and muscle balance. Overall, adopting these exercise routines can enhance circulation and reduce the likelihood of cramps occurring at night.
Managing Existing Cramps
Managing existing leg cramps is critical, especially for individuals who experience frequent nocturnal episodes. These muscular contractions not only cause discomfort but can also lead to disrupted sleep patterns. Addressing cramps through effective strategies can significantly enhance quality of life.
Immediate Relief Techniques
When confronted with a leg cramp, immediate relief is paramount. Several techniques can help alleviate the symptoms quickly:
- Stretching the Affected Muscle: Gently stretch the muscle that is cramping. For calf cramps, standing on a flat surface and slowly leaning forward with the affected leg straight may help. This action elongates the contracted muscle, providing immediate relief.
- Massage: Applying pressure to the cramped area can ease the pain significantly. Use your hands to rub the muscle gently, stimulating blood flow and promoting relaxation.
- Heat Therapy: Applying a warm compress or heating pad to the muscle can reduce cramping. The warmth eases tension, enhancing blood circulation to the area.
- Cold Therapy: In some cases, a cold pack can be useful. The cold reduces inflammation and numbs the area, providing temporary relief.
"Immediate attention to leg cramps can prevent the discomfort from escalating, allowing for a quicker return to restful sleep."
It is essential to try these techniques as soon as the cramp occurs. Timing is crucial in managing the pain effectively.
Long-term Management Strategies
To reduce the frequency and intensity of leg cramps over time, incorporating long-term management strategies is advisable:
- Regular Hydration: Maintaining proper fluid balance is fundamental. Drink sufficient water throughout the day to reduce the risk of dehydration, a known contributor to muscle cramps.
- Electrolyte Balance: Monitor and manage your electrolyte intake. Consuming foods rich in potassium, magnesium, and calcium promotes muscle health. Examples include bananas for potassium and dairy products for calcium.
- Adequate Warm-up and Cool-down: If you engage in physical activities, ensure that you perform proper warm-ups before exercising and cool-downs afterward. These practices prepare your muscles for activity and help in their recovery.
- Regular Stretching Exercises: Implementing stretching routines, particularly before bedtime, may help minimize the occurrence of night cramps. Focusing on legs and feet can be beneficial, allowing muscles to relax and remain flexible.
- Adequate Nutrition: A balanced diet is vital for muscle function. By ensuring sufficient intake of key nutrients, the body can maintain muscle integrity, reducing the likelihood of cramps.
Implementing these long-term strategies may take time but can lead to lasting benefits in managing leg cramps effectively.
When to Seek Medical Advice
Recognizing when to seek medical advice regarding late night leg cramps is essential for proper management and understanding of underlying issues. While occasional cramps are common, persistent or severe symptoms can indicate more serious health complications. An awareness of the signs and the right steps to take can make a significant difference in addressing this discomfort effectively.
Signs of Serious Underlying Issues
Late night leg cramps can sometimes hint at serious medical conditions. Various indicators may signal that professional evaluation is warranted. Among these signs:
- Severe Pain: Intense cramping that does not resolve quickly.
- Swelling: Noticeable swelling in the affected leg.
- Persistent Symptoms: Cramps occurring regularly over several nights.
- Skin Changes: Color or temperature changes in the leg.
- Numbness or Weakness: Difficulty moving the leg or experiencing numbness.
If these symptoms arise, it is crucial to consult a healthcare professional to ensure that there is no underlying vascular or neurological problem.
Consulting Specialists
When dealing with leg cramps, you may want to consult different types of specialists. Start with a primary care doctor who can evaluate your situation. If necessary, the doctor may refer you to:
- Neurologists: For evaluating nerve function or conditions affecting muscle control.
- Vascular Specialists: If there are concerns about blood flow issues.
- Dietitians: To assess nutritional deficiencies that could be contributing to cramps.
Seeking timely expert advice can lead to proper diagnosis and treatment. Being proactive in managing leg cramps ensures that you safeguard overall health as well as quality of sleep, reducing the risk of potentially serious complications moving forward.
"Taking early action by seeking medical advice can prevent future health issues related to leg cramps."
Ending
In the realm of late night leg cramps, understanding their causes is vital for effective management and prevention. This article meticulously outlines various factors that lead to these involuntary muscle contractions, emphasizing the multifaceted nature of the problem. From dehydration and nutritional deficiencies to underlying health conditions and lifestyle habits, each element contributes to the overall complexity of leg cramps.
Summarizing Key Points
The discussion highlights several key aspects:
- Physiological mechanisms: A thorough understanding of how muscles work is essential to grasp the roots of cramping.
- Impact of hydration and electrolytes: Staying hydrated and maintaining electrolyte balance is crucial for muscle function and reduces the risk of cramps.
- Lifestyle factors: Sedentary behavior and poor sleeping positions can exacerbate the likelihood of experiencing cramps at night.
- Health considerations: Conditions such as diabetes or peripheral artery disease significantly influence muscle health and may lead to cramping.
Proper knowledge enables individuals to adopt necessary strategies to mitigate discomfort.
Encouragement for Proactive Management
Proactive management of late night leg cramps can significantly enhance quality of life. Health professionals and wellness coaches should encourage strategies that incorporate:
- Regular hydration: Emphasize the importance of fluid intake throughout the day, especially for individuals at risk of dehydration.
- Balanced nutrition: Focus on diets rich in key nutrients like potassium, magnesium, and calcium to support muscle function.
- Exercise and stretching: Incorporate regular physical activity and specific stretches to increase flexibility and strength in leg muscles.
- Awareness of symptoms: Educate readers to recognize signs of cramping early, so they can respond effectively.
Overall, taking proactive steps will not only help in managing leg cramps but also contribute to overall well-being, allowing individuals to enjoy restful nights without the disruption of cramps.



